Health surveillance assistants as intermediates between the community and health sector in Malawi: exploring how relationships influence performance
Abstract:
Background
There is increasing global interest in how best to support the role of community health workers (CHWs) in building bridges between communities and the health sector. CHWs’ intermediary position means that interpersonal relationships are an important factor shaping CHW performance. This study aimed to obtain in-depth insight into the facilitators of and barriers to interpersonal relationships between health surveillance assistants (HSAs) and actors in the community and health sector in hard-to-reach settings in two districts in Malawi, in order to inform policy and practice on optimizing HSA performance.
Methods
The study followed a qualitative design. Forty-four semi-structured interviews and 16 focus group discussions were conducted with HSAs, different community members and managers in Mchinji and Salima districts. Data were recorded, transcribed, translated, coded and thematically analysed.
Results
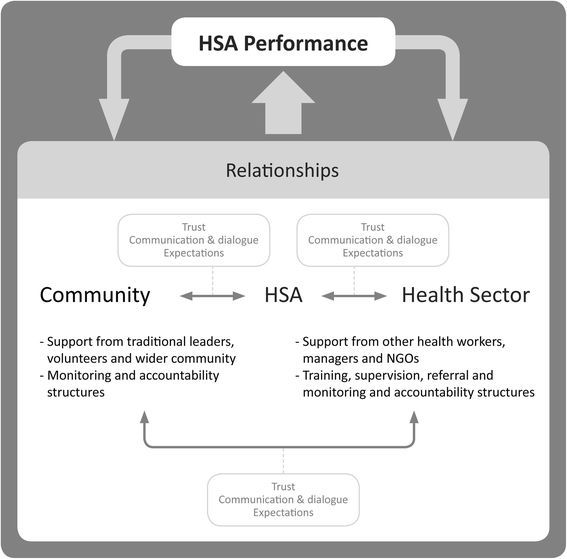
HSAs had relatively strong interpersonal relationships with traditional leaders and volunteers, who were generally supportive of their work. From the health sector side, HSAs linked to health professionals and managers, but found them less supportive. Accountability structures at the community level were not well-established and those within the health sector were executed irregularly. Mistrust from the community, volunteers or HSAs regarding incentives and expectations that could not be met by “higher levels” undermined support structures and led to demotivation and hampered performance. Supervision and training were sometimes a source of mistrust and demotivation for HSAs, because of the perceived disinterest of supervisors, uncoordinated supervision and favouritism in selection of training participants. Rural HSAs were seen as more disadvantaged than HSAs in urban areas.
Conclusions
HSAs’ intermediary position necessitates trusting relationships between them and all actors within the community and the health sector. There is a need to improve support and accountability structures that facilitate communication and dialogue, increase trust and manage expectations and thereby improve interpersonal relationships between HSAs and actors in the community and health sector. This would maximize the value of HSAs’ unique intermediary position and support them to deliver equitable health services. This is particularly important in rural areas, where HSAs often constitute the only point of contact with health services, yet report limited support from the health system.
Author: Maryse C. Kok, Ireen Namakhoma, Lot Nyirenda, Kingsley Chikaphupha, Jacqueline E. W. Broerse, Marjolein Dieleman, Miriam Taegtmeyer, Sally Theobald
Publication file: